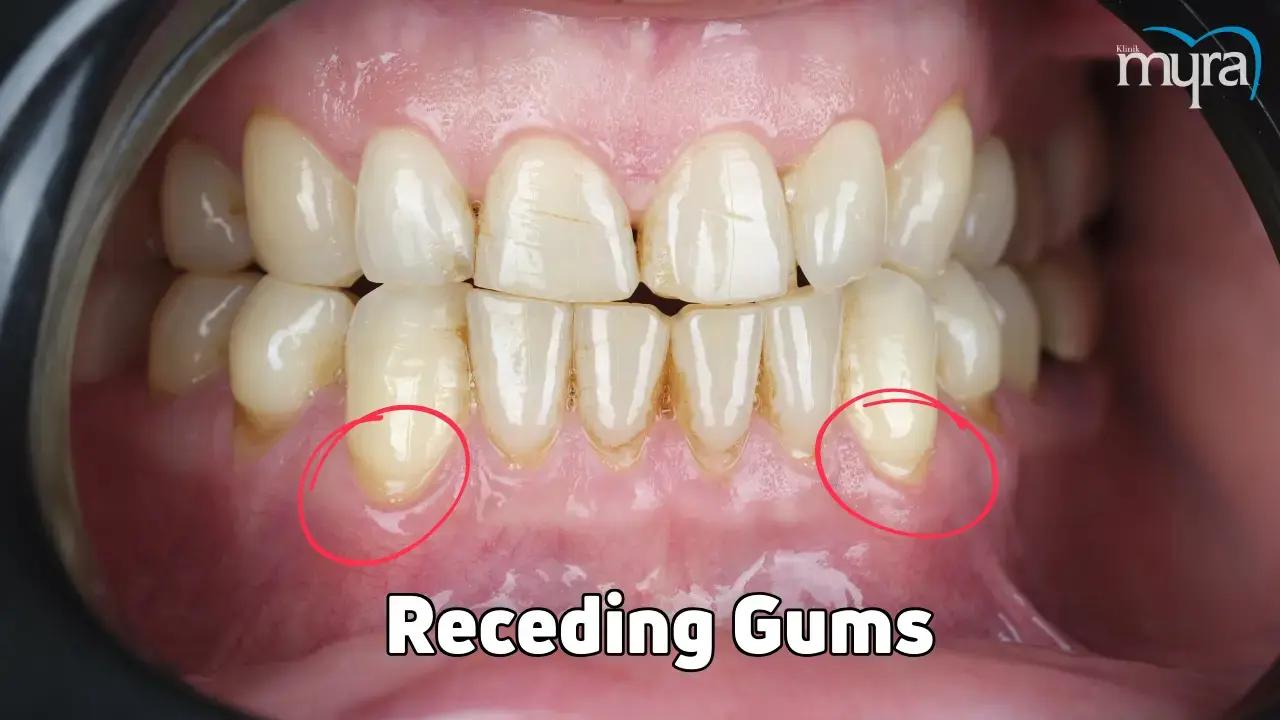
Receding gums (gingival recession) is a prevalent dental condition in which the gum tissue that envelops the teeth progressively shrinks or recedes, revealing a more significant portion of the tooth's root. Receding gums are classified based on the Miller Classification of Marginal Tissue Recession, and the types are Class 1, Class 2, Class 3, and Class 4. A gingival recession starts with moderate symptoms, such as gum irritation and slight bleeding when brushing or flossing. Patients observe changes in their gum line as the condition worsens, including a noticeable shrinkage of the gums and eventual exposure of the tooth roots. Patients at risk for receding gums must know the symptoms, treatment, and causes to attain preventive measures and seek professional help.
Symptoms of receding gums include persistent bad breath, red and swollen gums, bleeding after brushing or flossing, discomfort at the gum line, visibly shrinking gums, exposure of tooth roots, and loosening teeth. These indicators reflect the progressive character of gum recession and the underlying periodontal issues that require intervention.
The severity and specific requirements of the patient determine the treatment options for receding gums. Nonsurgical treatments include topical antibiotics to combat bacterial infection, dental bonding to conceal exposed roots, orthodontics to realign teeth and rebalance forces on the gums, and gum graft surgery to replace lost gum tissue and safeguard exposed roots.
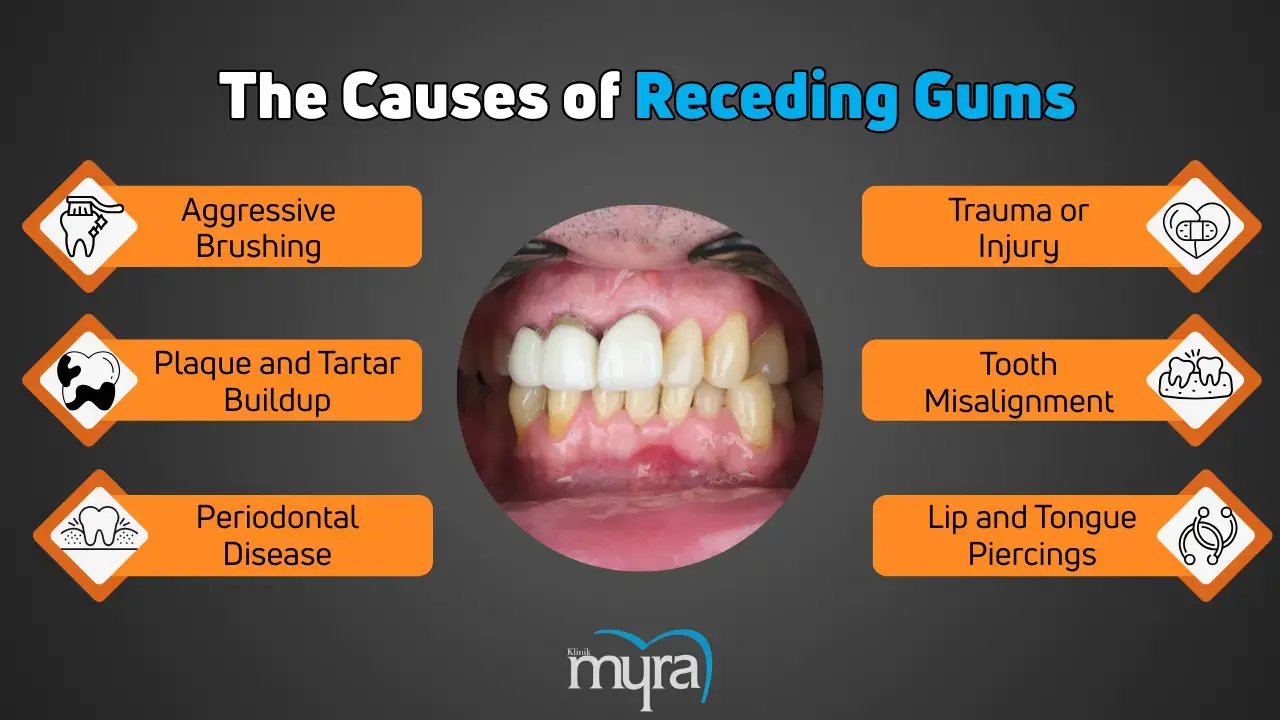
Causes of receding gums include aggressive brushing habits, which structurally alter the gums over time. Plaque and tartar buildup along the gumline leads to inflammation. Advanced periodontal disease destroys gum and bone tissues. Trauma or injury to the gums causes recession. Tooth misalignment puts uneven pressure on the gums. Smoking or tobacco use impairs gum health, and irritation from lip or tongue piercings contributes to gum recession.
"Treatment of Miller’s Class II Receding Gums Using Periosteal Reversal Technique," written by Kumar, et al., demonstrates the efficacy of periosteal reversal in achieving 95% root coverage for Miller's Class II recession over 12 months. "Gingival Recessions in Children (An Overview)," authored by Karimi, M., highlights diabetes, bruxism, and oral hygiene as key contributors to childhood gingival recession, advocating early preventive measures. "Association Between Gingival Recession and Its Biotype Among South Indian Population" by Vashita et al. identifies slender gingival biotypes as more prone to recession, suggesting interventions to thicken gingiva for prevention. "Gingival Recession on the Lingual Surface: Causes of Development," written by Khabadze, et al., examines tongue piercing, ankyloglossia, and lingual orthodontic appliances as significant factors in lingual gingival recession, emphasising preventive strategies based on a review of 134 studies.
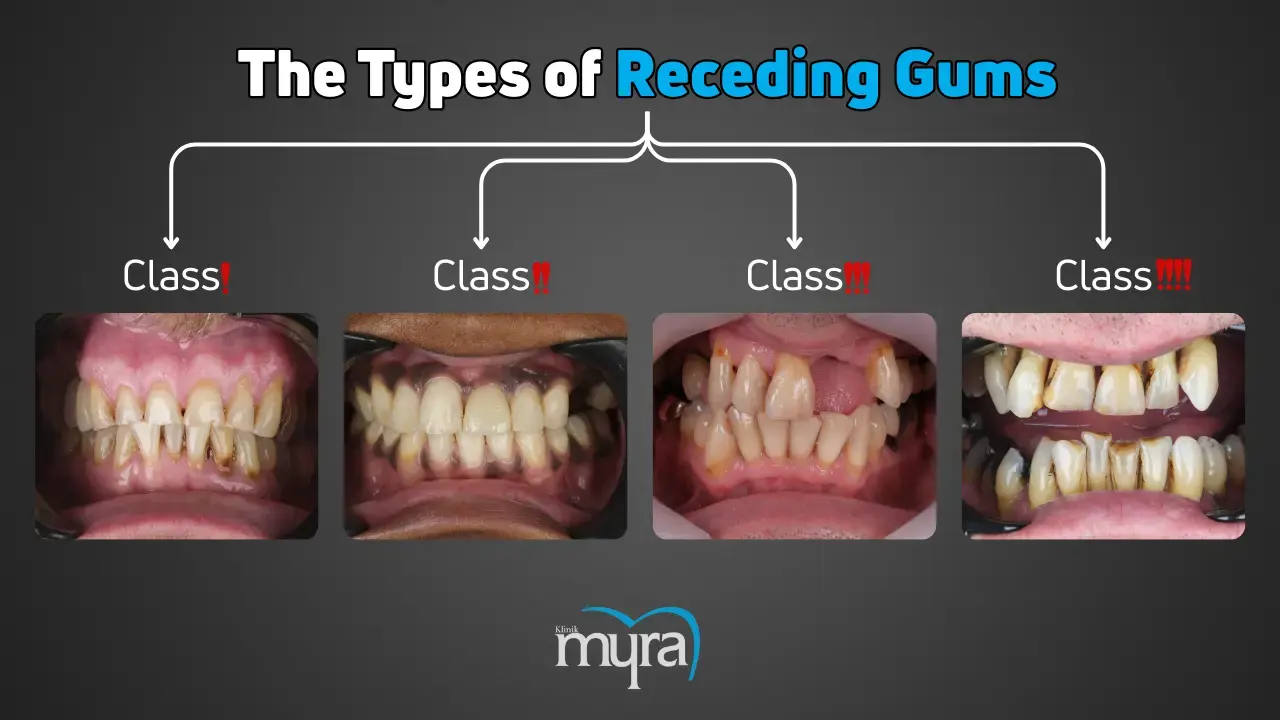
What are the Types of Receding Gums?
The types of receding gums are listed below.
Class 1 Recession: The class 1 recession is an initial-stage gingival recession with minimal soft tissue loss and no interdental bone loss. Targeted treatments have the potential to provide complete root coverage, as the gingiva remains securely attached to the tooth's facial surface.
Class 2 Recession: Class 2 recession is similar to Class 1, but the gingiva is dislodged from the tooth's facial surface despite intact interdental bone. Comprehensive root coverage is feasible with suitable interventions despite detachment.
Class 3 Recession: Class 3 recession is a substantial soft tissue and interdental bone loss, resulting in tooth displacement. Complete root coverage is more complex, while partial coverage is achieved in milder cases.
Class 4 Recession: Class 4 recession is a significant loss of soft tissue and interdental bone and the absence of a papilla between teeth.
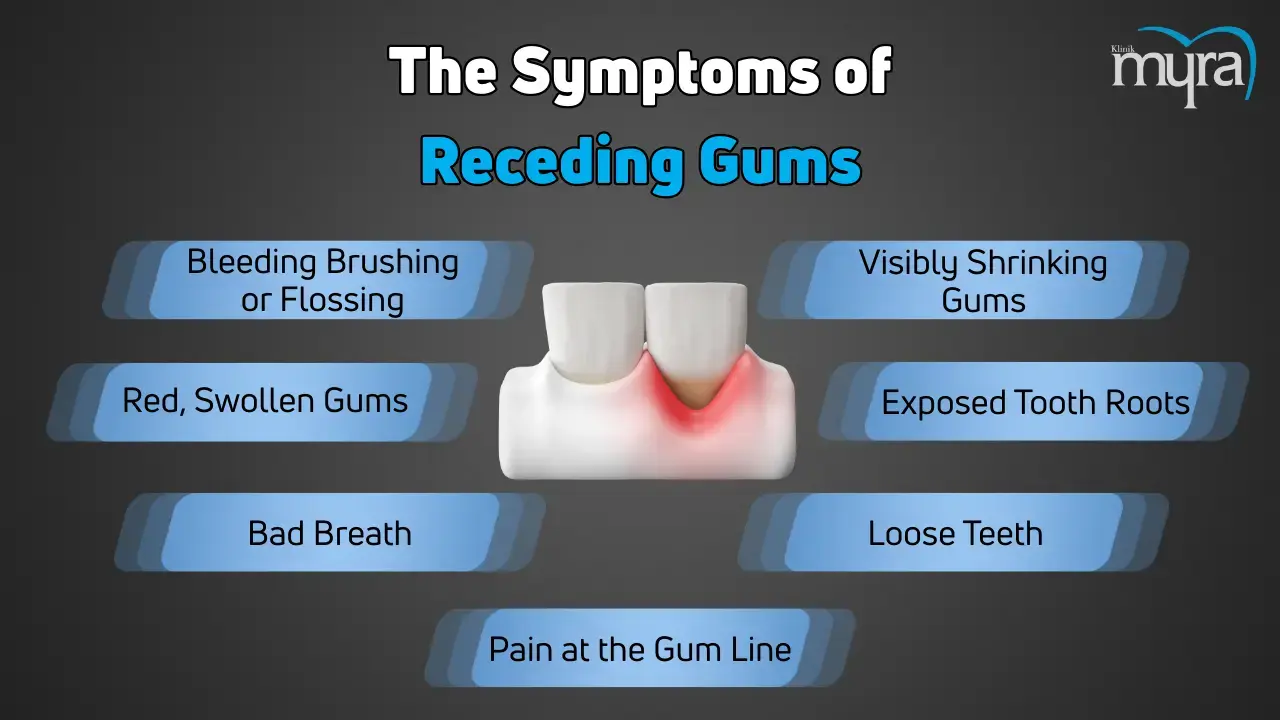
What are the Symptoms of Receding Gums?
The symptoms of receding gums are listed below.
Bleeding Following Brushing or Flossing: Bleeding during oral hygiene practices suggests gingivitis, a preliminary phase of receding gums. Gingivitis induces inflammation, compromising gum tissues and making them susceptible to bleeding when brushing or flossing.
Red, Swollen Gums: Red, swollen gums occur when the immune system reacts to microorganisms found in plaque and tartar that accumulate along the gumline. The immunological reaction increases blood circulation to the gums, resulting in visible inflammation and swelling, which are early indications of gingivitis.
Bad Breath: Halitosis (foul breath) is caused by the buildup of germs in plaque and tartar on the teeth and gums. The bacteria emit volatile sulfur compounds, which provide an unpleasant smell that contributes to halitosis, mainly when oral hygiene habits are insufficient.
Pain at the Gum Line: Gum disease progression from gingivitis to periodontitis causes increased inflammation and infection in the gum tissues and nearby bone. It leads to sensitivity and pain along the gum line, indicating more progressed stages of gum disease.
Visibly Shrinking Gums: Periodontitis, an advanced gum disease, leads to the slow erosion of gum tissue and underlying bone due to continuous inflammation. Gum recession occurs due to erosion, causing the gums to recede and uncover a more significant portion of the tooth's root structure.
Exposed Tooth Roots: Exposed tooth roots develop when receding gums leave the sensitive surfaces of the roots unprotected. The surfaces lack gum tissue to protect them from plaque buildup, which increases tooth sensitivity, decay, and eventual tooth loss risk if left untreated.
Loose Teeth: Severe periodontitis leads to substantial bone loss around the teeth, which weakens the structures that support them. Bone loss results in teeth becoming loose or movable, resulting in discomfort, difficulties in chewing, and tooth loss if not promptly addressed by a dental specialist.
What are the Causes Receding Gums?
The causes of receding gums are listed below.
Aggressive Brushing: Brushing with excessive force damages the delicate gum tissue, leading to gradual erosion and recession. Recession worsens over time due to the abrasion weakening the gums' bond to the teeth.
Plaque and Tartar Buildup: Bacterial plaque accumulates along the gumline and hardens into tartar, triggering an inflammatory response. The chronic inflammation causes the gums to pull away from the teeth, resulting in recession as the supporting structures are compromised.
Periodontal Disease: Advanced periodontal disease, or periodontitis, involves bacterial infection that destroys gum tissue and bone supporting the teeth. The gums recede and expose the tooth roots as the infection worsens, aggravating bone loss.
Trauma or Injury: Physical trauma to the gums, whether from accidents, dental procedures, or habitual behaviours, directly damages gum tissue. The trauma weakens the gum's attachment to the teeth, contributing to recession over time.
Tooth Misalignment: Misaligned teeth exert abnormal forces on the gums during chewing and biting. The excessive force leads to localised gum recession where the pressure is concentrated.
Smoking or Tobacco Use: Tobacco use impairs blood circulation and weakens the immune system in the gums, making them more susceptible to infection and inflammation. The chronic inflammatory response contributes to gum recession over time.
Lip and Tongue Piercings: Jewelry in oral piercings continuously rub against the gums, causing irritation and mechanical trauma. The established irritation leads to localised gum recession around the piercing site as the gum tissue recedes from the constant friction and pressure.
What are the Treatments of Receding Gums?
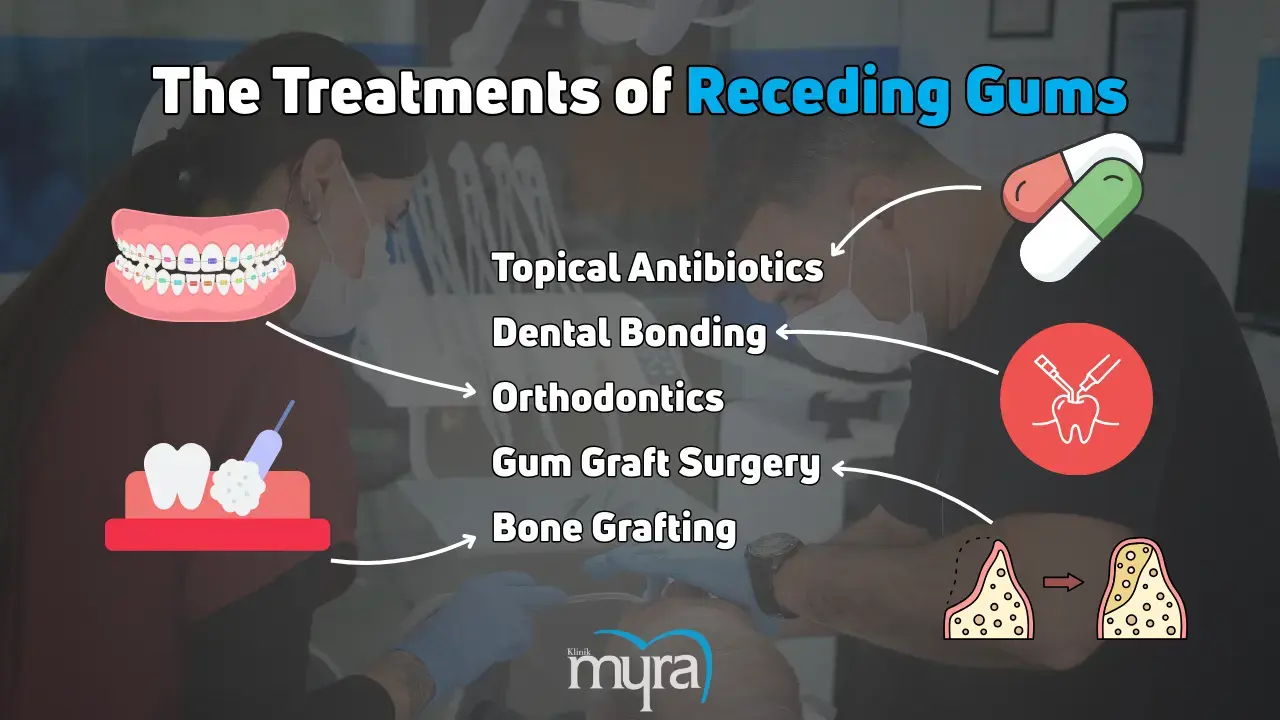
The treatments of receding gums are listed below.
Topical Antibiotics: Tropical antibiotics are administered directly beneath the gum line to address the deep-seated bacterial infections linked to gum disease, which is the primary cause of gum recession. Topical antibiotics target and eradicate harmful bacteria to promote gum healing and slow the advancement of recession by treating the underlying illness.
Dental Bonding: Dental bonding involves using tooth-coloured composite resin to conceal exposed tooth roots impacted by gingival recession. The procedure improves the cosmetic appearance and reduces root sensitivity by establishing a protective barrier against bacterial infiltration and external stimuli.
Orthodontics: Using braces or other orthodontic treatments to rectify tooth misalignment contributes to gum recession due to the uneven force distribution during biting and chewing. Orthodontics potentially reduces recession over time by realigning teeth and encouraging gingival tissue to realign and apply more balanced pressure to the gums.
Gum Graft Surgery: Gum graft surgery entails transplanting healthy gum tissue obtained from the mandible to regions where gum recession has occurred. Gum graft surgery offers long-term protection against further recession and improves gum health by restoring lost tissue volume and covering exposed tooth roots. The optimal results with minimal invasiveness are achieved by employing various techniques tailored to the patient's specific requirements and severity.
Bone Grafting: Bone grafting is required in extreme situations if a substantial loss of bone accompanies gum recession. The surgery entails transplanting bone tissue to the afflicted location to promote bone regeneration and give the teeth a strong foundation. Bone grafting and gum graft surgery are done together to guarantee that the recession and underlying bone loss are fully treated.
Can Receding Gums Be Treated At Home?
No, receding gums cannot be treated at home. A dentist must be seen by a patient for proper treatment and to prevent further recession, even though some home treatments and practices help control symptoms and improve gum health. Proper oral hygiene practices, such as brushing twice daily with a soft-bristled toothbrush and using delicate, circular motions to avoid abrasive brushing that exacerbates gum recession, are home care measures that support gum health. Fluoride toothpaste preserves oral health and reinforces tooth enamel.
Gum disease risk progression is reduced by regularly removing plaque and detritus between teeth and along the gum line through interdental cleaners or flossing. Mouth rinses with antibacterial ingredients, such as hydrogen peroxide, support oral hygiene by lowering the germs that cause gum inflammation and plaque development.
Professional dental care is required to address the advanced gingival recession. Dentists or periodontists suggest deep cleanings, such as scaling and root planing, to prevent bacterial reattachment and eliminate plaque and tartar below the gum line to smooth root surfaces. Surgical procedures such as gum grafting are necessary in certain instances to preserve exposed tooth roots and restore gum tissue lost due to recession.
What are the Researches about Receding Gums?
The researches about receding gums are about evaluating the effectiveness of various treatments and identifying factors that contribute to gingival recession, including surgical techniques, genetic predispositions, and lifestyle factors like oral hygiene practices.
The research “Treatment of Miller’s Class II Receding Gums Using Periosteal Reversal Technique: A Case File” concentrated on the periosteal reversal technique as a treatment for Miller's Class II receding gums. The process entails creating a partial-thickness membrane designed to reflect the periosteum. The flap is reversed to cover the exposed root surfaces of the afflicted teeth. The patient's gums at teeth #11 and #21 showed 5.1 mm and 4.8 mm of receding during the trial. The significant improvements observed after 12 months, specifically the 95% root coverage, demonstrated the procedure's potential to treat gingival recession effectively.
The research “Gingival Recessions in Children (An Overview)” emphasises the significance of periodontal health in children. It investigates the numerous factors contributing to gingival recession, including diabetes, bruxism, inadequate oral hygiene, malocclusions, and poor brushing techniques. The study emphasises the importance of establishing proper oral hygiene from a young age to prevent periodontal diseases. It explores potential treatment strategies without addressing specific clinical studies.
The study “Association Between Gingival Recession and Its Biotype Among South Indian Population- A Retrospective Study” analysed data from 86,000 patients to investigate the correlation between recession and gingival biotype in the South Indian population. The inclusion criteria were fulfilled by 106 patients out of the total. Patients with a slender gingival biotype were more susceptible to gingival recession, according to the analysis. The research shows that treatments that increase the thickness of the gingiva are good at preventing additional recession.
“Gingival Recession on the Lingual Surface: Causes of Development” was conducted to determine the causes of the gingival recession on the lingual surface. The recession development in the region was significantly influenced by factors such as tongue piercing, ankyloglossia, and the use of lingual orthodontic appliances. The study reviewed 134 articles and selected 55 that met specific inclusion criteria, emphasising the necessity of preventive measures and prospective interventions to reduce the risk associated with these factors.
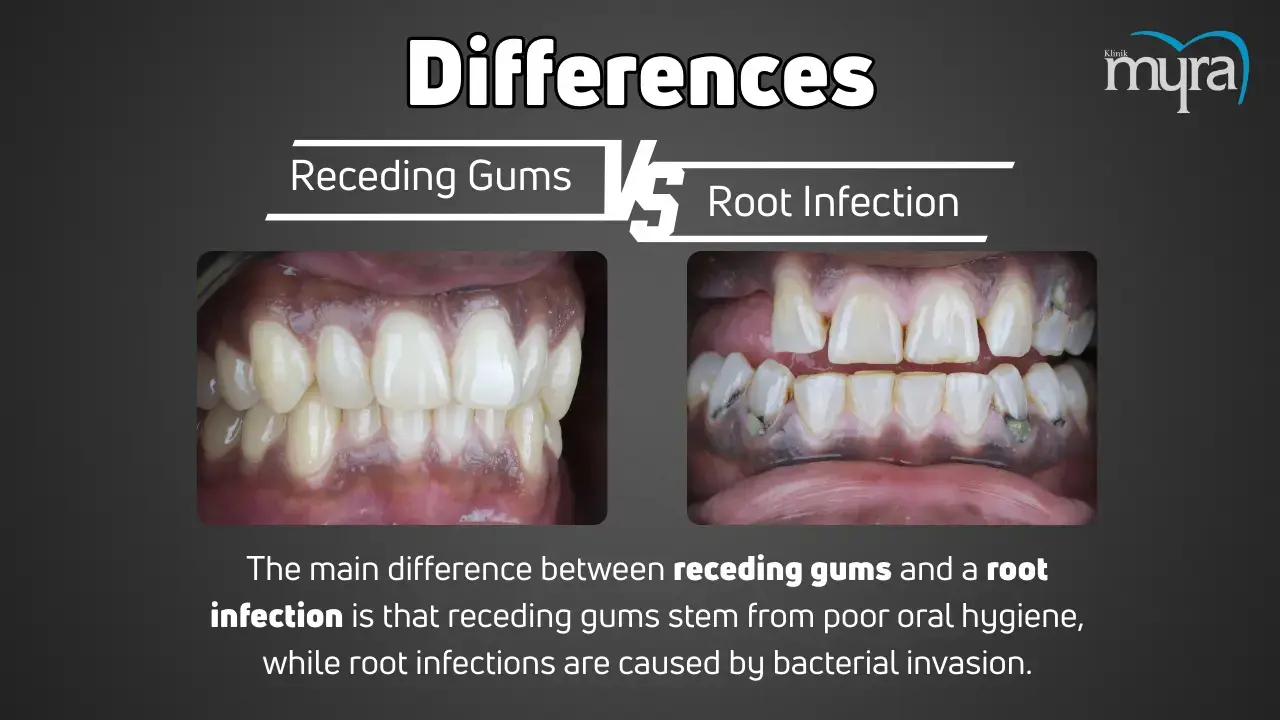
What are the Differences between Receding Gum and Root Infection?
The differences between receding gums and a root infection are notable in their causes and treatments. Receding gums happen when the gum tissue around the teeth fades away or pushes back, exposing more of the tooth or its root. The condition is caused by poor dental hygiene, vigorous brushing, periodontal disease, trauma or injury, and smoking or tobacco use. Treatments for receding gums target the underlying dental problem. Treatments include better oral hygiene practices, scaling, root planing, or surgical procedures such as gum grafts to replace lost tissue.
Root infections (abscessed teeth) are caused by a disease at a tooth's root or between the gum and the tooth. The infections are caused by untreated cavities, cracks, or chips in the tooth or dental trauma, which allows bacteria to enter the tooth's pulp and cause disease. A root infection is treated with treatments such as root canal therapy, which removes the infected pulp and cleans and seals the inside of the tooth. The affected tooth needs to be removed in extreme cases.
Receding gums and root infections are similar because they cause substantial discomfort and severe consequences if not treated. Symptoms such as tooth sensitivity, pain, and oedema occur in disorders. Regular oral hygiene is essential for avoiding and treating receding gums and root infections. The main distinction is that receding gums are caused by gum tissue problems and poor dental hygiene, whereas root infections are caused by bacterial invasion of the tooth pulp.