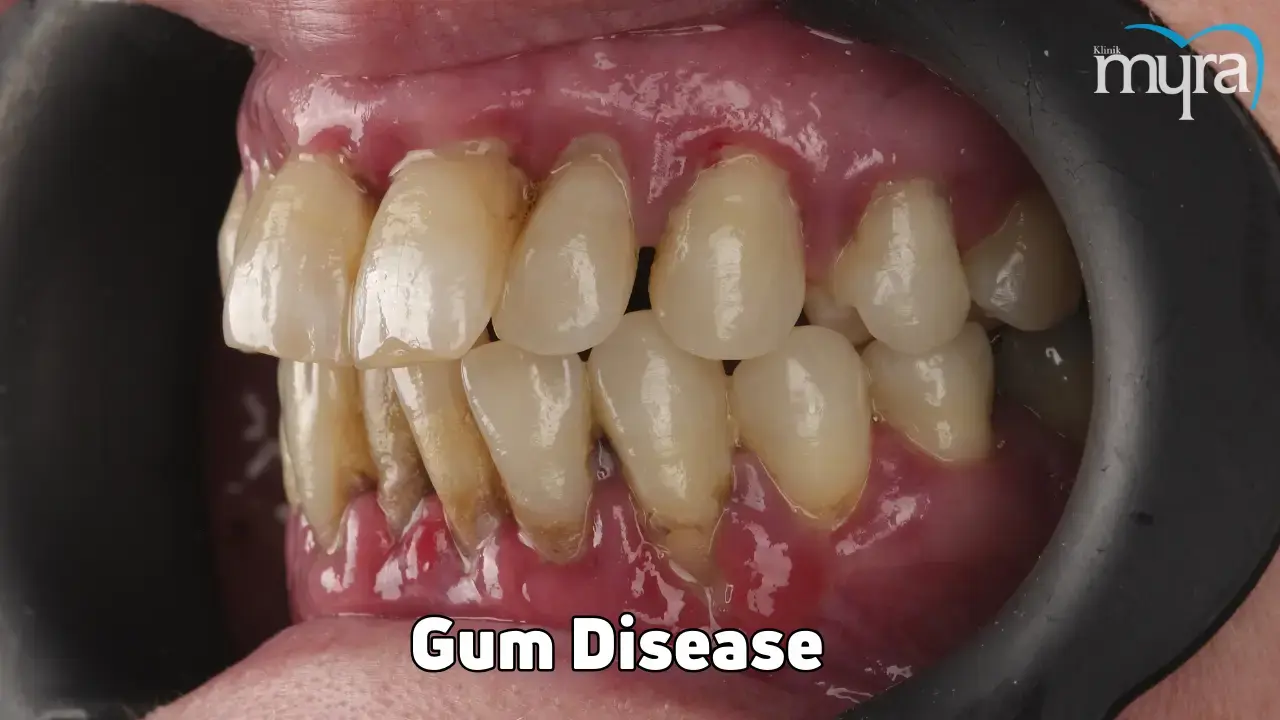
Gum disease is an infection caused by poor brushing and flossing habits that damages tooth soft tissue, leading to tooth loss. Understanding gum disease symptoms, treatment, and causes helps maintain health and well-being. Early detection allows for prompt treatment, reducing the risk of severe complications. Prevention involves understanding the causes of gum disease and the effective treatment options available to restore gum health and prevent future invasive procedures.
Gum disease symptoms include swollen or puffy gums, tender gums, bleeding when brushing or flossing, pus between teeth and gums, and changes in teeth alignment. Untreated inflammation leads to tooth decay and loss. Proper treatment is crucial for reversible gum disease. Tender gums occur when poor oral hygiene causes inflammation, causing discomfort and redness. Gum bleeding is a reversible condition. Body plaque (tartar) is the cause of gum bleeding. A puss between teeth and gums indicates a gum abscess. Teeth alignment changes due to infection and toxins.
Gum disease treatments include antibiotics, soft tissue grafts, bone grafts, tissue-stimulating proteins, and scaling and root planing. Topically or orally administering antibiotics controls infections and reduces inflammation. Soft tissue grafts cover visible roots and restore gum tissue, while bone grafts restore lost bone around teeth due to periodontitis. Tissue-stimulating proteins stimulate healthy bone and tissue growth, promoting cell proliferation and tissue repair. Scaling and root planing are dental procedures that remove tartar and smooth tooth surfaces, while gum contouring is a cosmetic dental procedure to improve gum appearance.
Poor oral hygiene, smoking, certain medications, a poor diet, diabetes, hormonal changes, genetics, and immunodeficiency cause gum disease and dental problems. Poor oral hygiene leads to plaque, tartar, gingivitis, periodontitis, tooth mobility, and tooth loss. Smoking, certain medications, a poor diet, and hormonal changes during periods such as puberty, pregnancy, menstruation, and menopause increase the risk of gum disease. Smoking causes dry mouth and gum overgrowth, while a poor diet leads to tooth decay and nutrient deficiencies.
The differences between gum disease and tooth decay are that gum disease is an infection and inflammation of gums and tooth structures, while tooth decay is bacteria-induced tooth enamel and structure degradation. Gum disease and tooth decay are oral health issues caused by bacteria, causing inflammation and eroded enamel. Risk factors include smoking, diabetes, poor oral hygiene, and genetics. Treatment involves regular cleanings, brushing, and dental cleanings.
The research on gum diseases is gum tissue regeneration, linking gum disease with cancer and dementia. Dr Nigel Carter's study combines biological and mechanical techniques to repair and regenerate bone and gum tissue, preventing tooth loss and restoring oral health. A study led by Drs. Zepeda Rivera, Susan Bullman, and Christopher D. Johnston found that Fusobacterium Nucleatum, is linked to colorectal cancer. Targeting Fna C2 in colorectal tumours improves patient outcomes. The National Institutes of Health (NIH) study indicates that gum disease-causing bacteria are linked to dementia with oral infection preceding dementia diagnosis, highlighting the need for clinical trials.
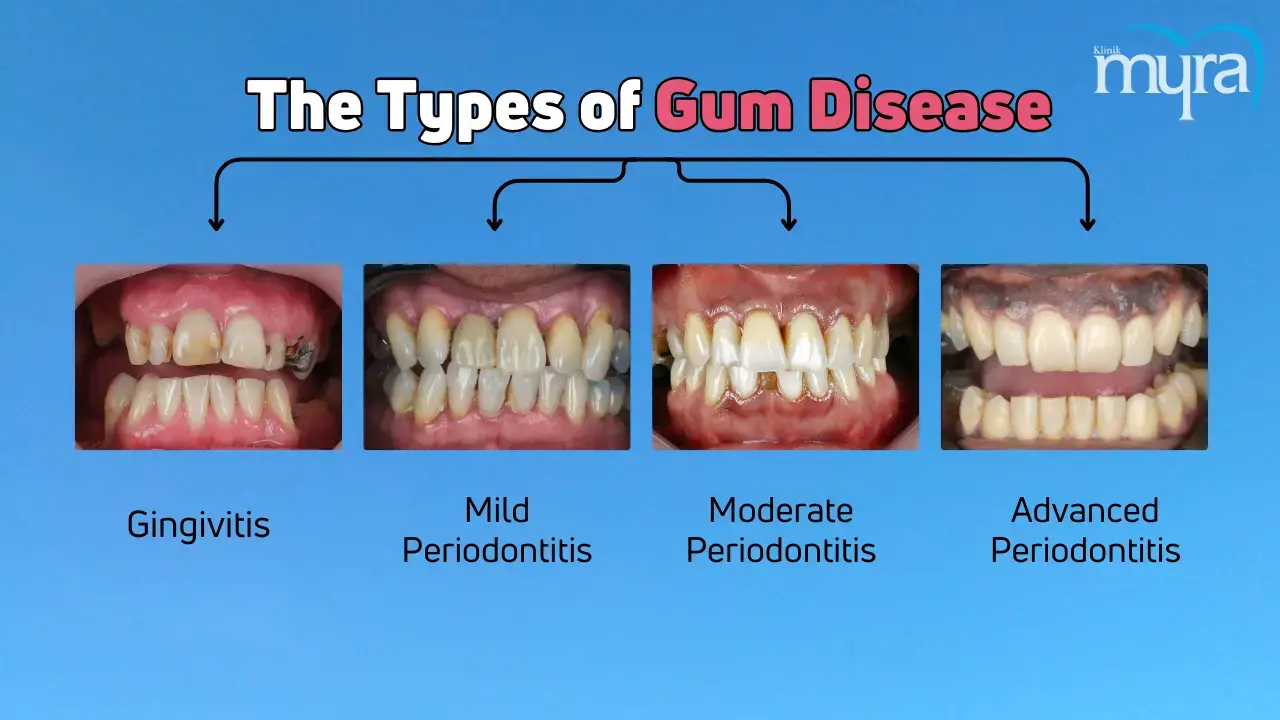
What are the Types of Gum Disease?
The types of gum diseases are listed below.
Gingivitis: Gingivitis is a mild periodontal condition inducing inflammation of the gums around the base of teeth. Symptoms of gingivitis comprise red, swollen, and tender gums, which bleed easily during daily cleanings and flossing. Poor oral hygiene contributes to the formation of bacterial plaque, which is the cause gingivitis. Risk factors include hormonal transformations, smoking, family history, medications, diseases, ageing, and viral and fungal infections. Preventative measures include brushing and flossing twice daily, using fluoride toothpaste, maintaining a balanced diet, and regular dental cleanings.
Mild Periodontitis: Mild periodontitis is a phase of gum infection that occurs after untreated gingivitis. It causes the gums to pull away from the teeth, forming periodontal pockets and involves bone loss and eroded tooth tissues. Symptoms include reddish or purplish gums, swollen gums, bleed-like gums, bad breath, pus around the gum line, loose teeth, tooth loss, gum recession, and chewing pain. It is caused by poor oral hygiene, which clings to plaque and tartar on tooth surfaces.
Moderate Periodontitis: Moderate periodontitis is an advanced stage of gum disease characterised by increased inflammation. It has symptoms such as bacteria adhering to plaque and tartar on tooth surfaces, causing infection, bone loss, and tooth loss. Symptoms include reddish, purplish, swollen, tender gums, bleed-like gums, bad breath, pus around the gum line, loose teeth, pain when chewing, new spaces between teeth, and gum recession.
Advanced Periodontitis: Advanced periodontitis is the most severe stage of gum disease, characterised by inflammation, infection, and extensive damage to the gums and supporting structures of the teeth. It results in the deepening of periodontal pockets, where plaque, tartar, and bacteria accumulate. The advanced periodontitis stage leads to substantial bone loss around the teeth, which causes additional complications if not treated promptly. Poor oral hygiene erodes tooth support tissues.
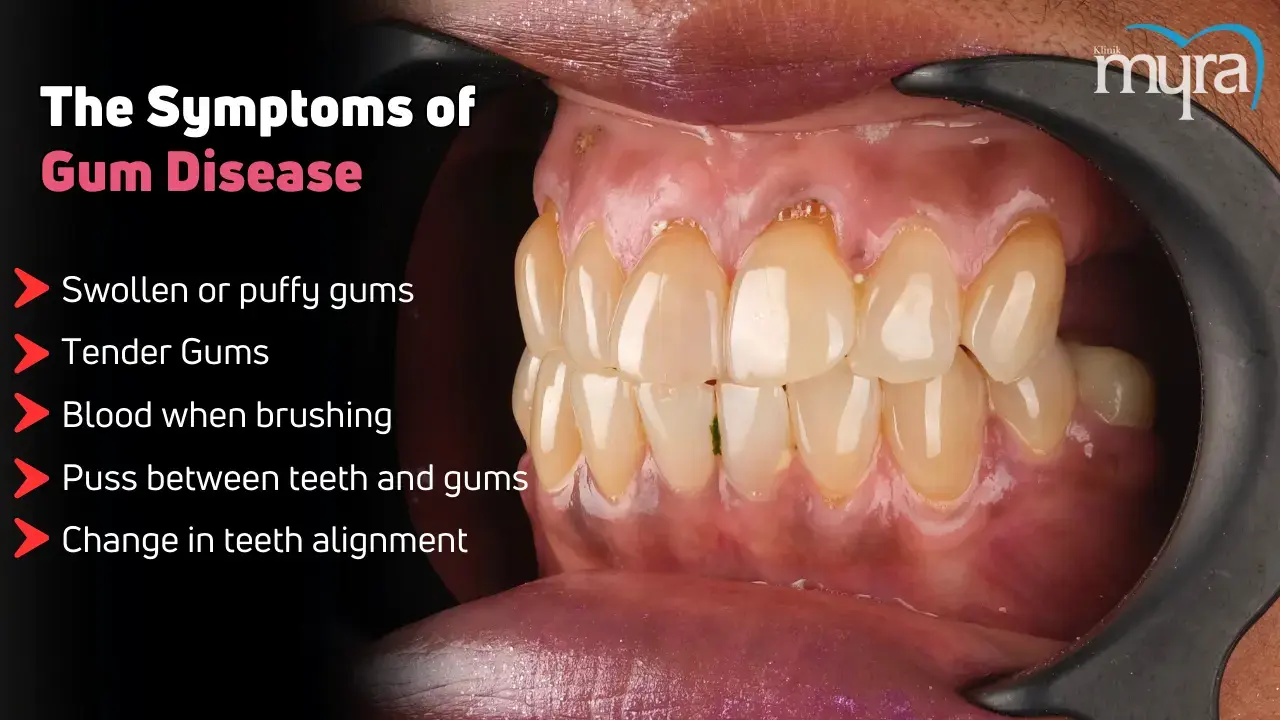
What are the Symptoms of Gum Disease?
The symptoms of gum disease are listed below.
Swollen or puffy gums: Swollen or puffy gums are signs of gum disease, including periodontitis and gingivitis. Inflammation from poor dental hygiene causes swollen, red, and bleeding gums. Untreated inflammation leads to severe symptoms, tooth decay, and loss.
Tender Gums: Tender gums happen when poor oral hygiene leads to inflammation in the gums, causing discomfort and other symptoms such as redness, swelling, and bleeding. The immune response to the bacteria causes the area to become inflamed and tender.
Blood when brushing or flossing: Gum bleeding is a cause of periodontal disease, which is reversible with proper treatment. Bacterial plaque, or tartar, lodged under the gum tissue causes inflammation. Persistent bleeding when brushing or flossing indicates the need for dental care.
Puss between teeth and gums: Puss between teeth and gums is a symptom of gum abscess. It occurs when bacteria from the mouth invade the space between the teeth and gums, leading to an infection in the surrounding tissue. The infection results in the formation of an abscess, a pocket filled with pus. The presence of pus indicates that the body is trying to fight off the infection.
Change in teeth alignment: Teeth alignment changes due to various factors, including the loss of jawbone density, changes in gum tissue, and advanced gum disease, specifically periodontitis. The infection in gingivitis spreads deeper into the supporting structures of teeth, including the periodontal ligament and alveolar bone. The bacteria produce toxins that trigger an inflammatory response, damaging the periodontal tissues, including the bone holding teeth in place.
What are the Causes Gum Disease?
The causes of gum disease are listed below.
Poor oral hygiene: Poor oral hygiene is a condition in which the mouth is not kept clean and disease-free. It leads to plaque formation, tartar formation, gingivitis, periodontitis, tooth mobility, and tooth loss. Poor oral hygiene causes tooth decay, bad breath, tooth staining, tooth sensitivity, and oral infections.
Smoking: Smoking affects oral health through reduced blood flow, impaired immune response, increased plaque and tartar build-up, and impaired healing capacity. The toxins in tobacco smoke directly damage gum tissue, leading to inflammation and degradation. Smokers' damaged gums do not heal as effectively as non-smokers', and their inflammatory response leads to chronic inflammation. Smoking causes dry mouth, as less saliva helps wash away food particles and bacteria. It alters the pH balance in the mouth, creating an environment that supports the growth of pathogenic bacteria.
Certain Medications: Certain medications increase the risk of developing gum disease by causing side effects that impact oral health. Side effects include reduced saliva production, gum overgrowth, and body immune response changes. Medications, such as antihistamines, decongestants, antidepressants, and blood pressure medications, cause dry mouth by reducing saliva flow, creating an environment where bacteria thrive, leading to plaque build-up and gum inflammation. Anticonvulsants, calcium channel blockers, immunosuppressants, and chemotherapy drugs cause gum overgrowth, plaque accumulation, and inflammation. Sugar-containing medications and hormonal changes in oral contraceptives contribute to gum disease and inflammation.
Poor Diet: A poor diet impacts oral health, leading to tooth decay, erosion of tooth enamel, and nutrient deficiencies. Tooth decay occurs when bacteria in the mouth feed on sugary foods or drinks, producing acids that attack tooth enamel. Acidic foods and beverages, such as citrus fruits and soda, erode tooth enamel over time, making teeth more susceptible to decay. Insufficient calcium and vitamin D lead to tooth decay. Dehydration results from inadequate water, leading to dry mouth and an increased risk of tooth decay and other oral health problems.
Diabetes: Diabetes contributes to gum disease through increased glucose in saliva, reduced saliva production, high blood sugar levels, inflammation, and an impaired immune response. Diabetes impairs white blood cell function, slows healing, and increases glucose levels in saliva, leading to bacterial growth and plaque build-up. Reduced saliva production causes dry mouth and an increased bacterial load, making the mouth susceptible to infections.
Hormonal Changes: Hormonal changes in estrogen and progesterone contribute to gum disease by increasing blood flow to the gums, making them sensitive to inflammation, and affecting the body's response to plaque buildup. Estrogen and progesterone levels fluctuate during perimenopause, causing some anti-inflammatory protection to disappear. Hormonal changes during periods such as puberty, pregnancy, menstruation, and menopause increase the risk of gum disease, leading to swollen, bleeding gums, dry mouth, and altered taste.
Genetics: Genetics affects the susceptibility to gum disease through various mechanisms. Gum disease starts and worsens because of differences in immune responses, the health of connective tissues, the microbiome in saliva, inflammatory mediators, bone metabolism, and genetic syndromes. Genetic differences lead to hyperactive immune reactions, weaker gum tissues, and increased susceptibility to infection. Genetic syndromes, such as Down syndrome or Papillon-Lefèvre syndrome, increase the risk of severe gum disease due to their impact on the immune system and connective tissues.
Immunodeficiency: Immunodeficiency is a condition in which the immune system is impaired or dysfunctional, leading to reduced immune function and increased susceptibility to infections. It leads to gum problems, including inflammation and gum disease. Immunodeficiency compromises the immune system's ability to fight infections, regulate inflammation, and maintain a healthy oral environment. Immunodeficiency disorders are associated with systemic conditions or medications that indirectly affect gum health.

What are the Treatments of Gum Disease?
The treatments of gum disease are listed below.
Antibiotics: Bacterial plaque buildup around the teeth and gums is the root cause of gum disease, which requires antibiotics. Antibiotics are administered topically or orally and help control bacterial infections, enhance treatment effectiveness, and reduce inflammation. Oral antibiotics are prescribed for a specific duration, while topical antibiotics are applied directly to the gums during dental visits.
Soft Tissue Grafts: Surgical soft tissue grafts are used to treat gum disease that has caused gum recession and help fix it by covering visible roots and restoring gum tissue. Connective-tissue grafts involve cutting a flap of skin at the roof of the mouth, removing tissue from under the flap, and stitching it to the gum tissue surrounding the exposed root. Soft tissue grafting helps restore gum tissue, protect tooth roots, and enhance the function and aesthetics of the smile.
Bone Grafts: Bone grafting is a surgical procedure to restore lost bone around teeth due to periodontitis. It helps prevent tooth loss by holding the tooth in place and serving as a platform for the regrowth of natural bone. The procedure involves using a person's bone, donated bone, or synthetic bone to rebuild areas damaged by gum disease. The graft is a scaffolding that holds space until the body regenerates new bone.
Tissue-stimulating proteins: Tissue-stimulating proteins are a promising treatment for gum disease. It stimulates the growth of healthy bone and tissue, helping repair and regenerate damaged areas. The therapy combines surgical procedures, such as implanting a thin membrane between the gum and tooth to block infection and deliver antibiotics, medication, and growth factors, including tissue-stimulating proteins. Tissue-stimulating proteins help heal and regenerate damaged tissues, promoting cell proliferation, angiogenesis, and tissue repair.
Scaling and root planing: Scaling and root planing are dental procedures used to treat gum disease, involving deep cleaning with handheld instruments or ultrasonic devices. Scaling removes built-up tartar from teeth and gums, while root planing smooths tooth surfaces to prevent plaque and calculus reaccumulation. The procedure takes multiple visits and requires a post-procedure checkup. Gum contouring, or gum reshaping, is a cosmetic dental procedure performed after scaling and root planing to improve the appearance of the gums. It is recommended for people with excessive gingival display or uneven gum lines.

Can Gum Disease Be Treated At Home?
No, gum disease cannot be treated at home. Accurate diagnosis, remedy, and management demand professional dental cures. Dentists or periodontists assess the severity of gum disease through comprehensive oral exams, probing depths, and X-rays and determine the appropriate therapeutic plan. Recurring dental cleanings remove plaque, tartar, and bacteria from the teeth and gumline. Developed stages of gum disease, such as periodontitis, demand intensive remedies such as scaling and root planing.
Dentists prescribe prescription medications for gum disease-related bacterial infections, such as antibiotics or antimicrobial mouthwashes. Surgical interventions, such as flap surgery, bone grafts, or soft tissue grafts, require specialist and professional expertise. Regular follow-up visits with a dentist or periodontist help monitor treatment progress, evaluate healing, and adjust the treatment plan as needed. Natural remedies, such as neem extract mouthwash, clove oil, tea tree oil, and coconut oil, help manage periodontitis at home, though they are insufficient to treat the condition. Progressive impairment, professional cleaning, and an increased risk of systemic diseases are all needed to diagnose, treat, and manage gum disease properly.
What are the Researches about Gum Disease?
The research on gum diseases is about gum tissue regeneration, linking gum disease with cancer and dementia. A new study by Dr. Nigel Carter OBE has combined biological and mechanical techniques to repair and regenerate bone and gum tissue, preventing tooth loss and restoring oral health. Researchers implanted a thin membrane between the inflamed gum and tooth, blocking infection and delivering antibiotics, medication, and growth factors to the gum tissue. The treatment has the future of improving the quality of life for people affected by periodontitis, which leads to widespread health issues.
Drs. Martha Zepeda Rivera, Susan Bullman, and Christopher D. Johnston of the Fred Hutchinson Cancer Center led a research team for a study that received funding from the National Institutes of Health (NIH). The team found that Fusobacterium Nucleatum, a bacteria implicated in gum disease, is linked to colorectal cancer. The researchers found that Fna C2, a subspecies of Fna, was present in colorectal tumours. The bacteria trigger inflammation, leading to tooth loss and periodontal disease. The researchers suggest that targeting Fna C2 in colorectal tumours improves patient outcomes and identifies aggressive tumours.
A study by the National Institutes of Health (NIH) suggests that bacteria causing gum disease are linked to Alzheimer's disease, related dementias, and vascular dementia. The study used data from the National Health and Nutrition Examination Survey (NHANES) to compare the risk of gum disease and oral bacteria infections with dementia diagnoses and deaths. The findings suggest that oral infection precedes dementia diagnosis, and clinical trials are needed to test the effectiveness of treating diseases.
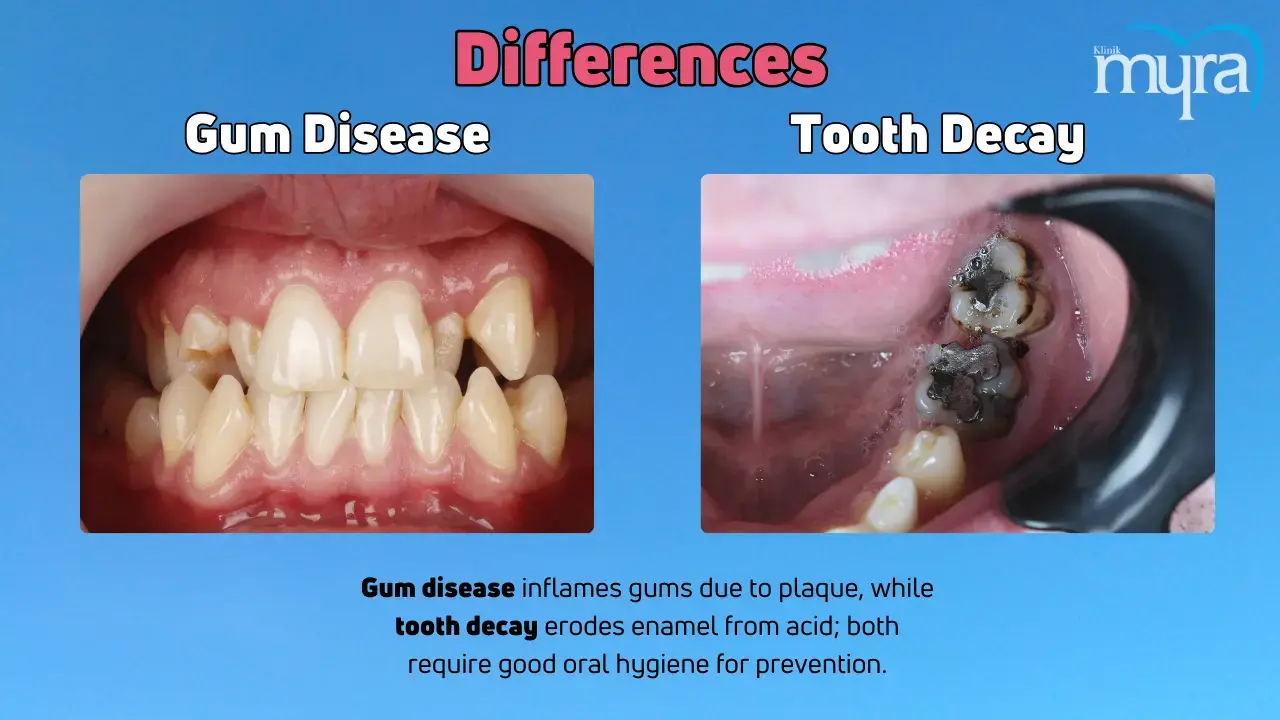
What are the Differences between Gum Disease and Tooth Decay?
The difference between gum disease and tooth decay is that gum disease is a condition that causes inflammation of the gums and tooth structures, while tooth decay is the breakdown of tooth enamel and structure by bacteria. Bacterial plaque collection around teeth causes gum infection, which advances to gingivitis and periodontitis. Risk factors include smoking, diabetes, inadequate oral hygiene, medication side effects, stress, genetics, malocclusion, clenching, or bruxism.
Bacteria in the mouth turn glucose into acid, which erodes tooth enamel and causes tooth decay. Plaque accumulation on teeth leads to increased acid production, causing tooth decay. Gum disease is treated with periodic dental cleanings and brushing, while tooth decay involves extracting decayed tooth parts and replacing them with fillings. Severe cases require deep cleaning, prescription mouth rinses, or periodontitis-related surgery.
Gum disease and tooth decay are oral health issues caused by bacteria. Gum disease causes inflammation of the gums, while tooth decay causes eroded enamel. They are prevented through good oral hygiene practices, including brushing, flossing, and dental cleanings. Gum disease causes red, swollen, and bleeding gums, while tooth decay causes toothache, sensitivity, and visible holes. Gum disease and tooth decay require professional restorative care, and aspects such as poor diet, smoking, certain medical ailments, and genetic predisposition increase the risk.